Uterine fibroma is a benign tumor, developed from the uterine muscle and consisting of smooth uterine muscle and fibrous tissue. Macroscopically, a fibroid is a hard, more or less rounded mass of variable volume. 20% of women over 35 years of age are affected by fibroids.
RISK FACTORS:
The formation mechanism is still not well known.
• There is a hormonal factor with an estrogen-promoting role. Thus during pregnancy and perimenopause, its volume increases.
• There is also an ethnic factor (common among black women)
• And a hereditary factor.
ITS LOCATION:
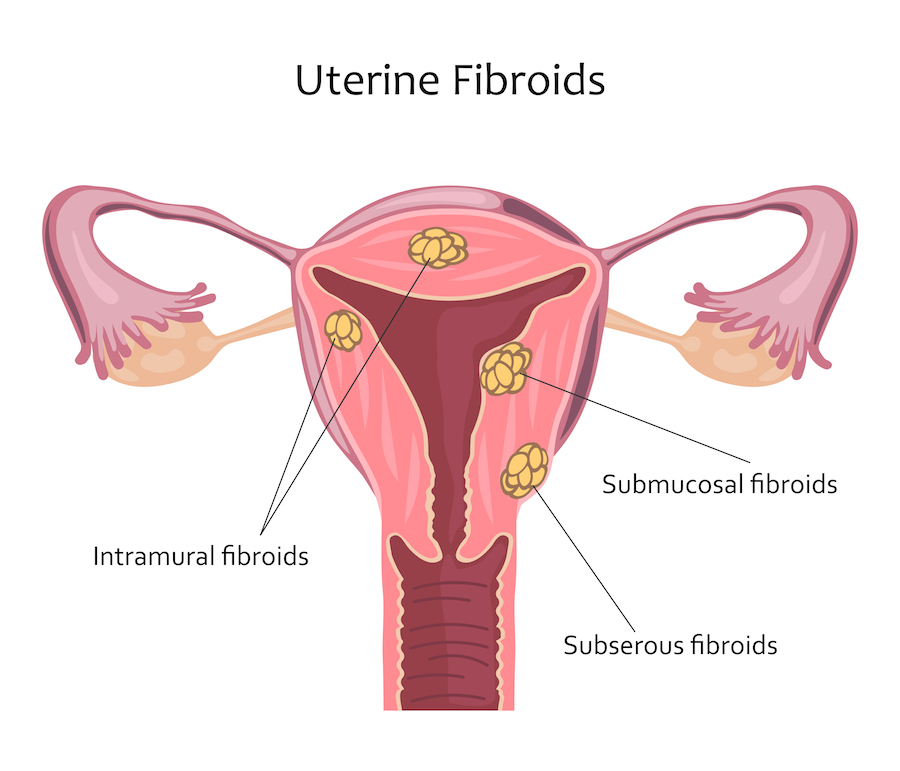
• Interstitial fibroma: develops in the thickness of the myometrium (muscle of the uterus) that it will deform
• Submucosal fibroma: develops under the endometrium, protrudes into the uterine city
• Intra-cavitary fibroma: located in the uterine cavity, it develops towards the uterine cervix
• Sub-serous fibroma (10% of cases): develops outside the uterus, under the serosa. It is often asymptomatic.
SYMPTOMS:
Often asymptomatic, of chance discovery during gynaecological examination.
Sometimes they are responsible:
• Menorrhagia: heavy and prolonged periods
• Urinary bladder compression disorders: permanent urge to urinate, stress incontinence
• Feeling of pelvic gravity
• Progressive and painless increase in the volume of the stomach.
Duration of hospital stay
2 to 4 days.
Average length of stay
7 to 10 days.
The doctor will ensure that the patient is stable before travelling.
Every year, nearly 11 million patients go abroad in search of medical care. At MEDICAIM, we provide our patients with access to the best hospitals and doctors around the world. Contact us to learn more about your treatment options.
Ask for your free quote abroad
Start your medical stay by requesting a quote. Our customer service department will help you find the clinic that best suits your needs and get you a quote.
DIAGNOSIS:
• On clinical examination, possibility of palpating the mass with a vaginal touch
• The cervico-vaginal smear is systematic
• Pelvic ultrasound confirms the diagnosis, makes it possible to specify its location and volume.
COMPLICATIONS:
They occur when the fibroids are asymptomatic:
• Compression of the bladder or rectum, if the fibroma is large, leading to urinary disorders and constipation
• Fibroid infections
• Fertility disorders
• Hemorrhages related to hormonal imbalance
• Anemia (decrease in hemoglobin levels due to lack of iron) as shown by a blood test.
Several types of treatments exist, asymptomatic fibroids are not treated.
Medical treatment:
The doctor gives:
• Progestins to limit bleeding disorders associated with fibroids
• LHRH agonists, which correspond to medical castration to reduce the volume of fibroma. It is prescribed preoperatively to facilitate the procedure.
Surgical treatment:
It is indicated in case of:
• Severe bleeding resistant to medical treatment
• Complicated fibroids
TWO SURGICAL POSSIBILITIES:
• By surgical hysteroscopy, fibroids developed in the uterine cavity (submucosal fibroids) are removed by endoscopy (small camera with scalpel) provided that their size is less than 4 cm.
• By laparotomy (the abdominal wall is opened) a myomectomy is performed:
The doctor removes fibroids developed outside the uterus (subserous fibroids) and in the uterine muscle (intramural fibroids) by cutting the muscle. Myomectomy may weaken the uterus and in some cases require a subsequent cesarean section.
A drain is placed to avoid any hematoma
The procedure involves incising the lining of the uterus, removing the fibroid(s) and closing the lining of the uterus. It requires general or local-regional anaesthesia (epidural, spinal anaesthesia).
The doctor performs a total hysterectomy: the entire uterus is removed; the ovaries and fallopian tubes are preserved in women under 50 years of age.
It can be done in three different ways:
• Through the vaginal route, leaving no visible scars.
• By laparoscopy, i. e. by inserting small tubes through the wall of the abdomen. There are small, very discreet scars on this level.
• By laparotomy, i. e. by opening the belly as is done for a caesarean section. This approach is reserved for large uteri or in case of failure of any of the other 2 approaches.
The procedure takes between 40 and 60 minutes.
The consequences of this intervention:
The cervix at the bottom of the vagina will be replaced by a simple painless scar. This does not affect the quality of sexual intercourse.
Impact of hysterectomy:
• Loss of fertility
• Stop menstruation without there being problems of weight and hot flashes because it is not a menopause, the eggs are still produced by the ovaries.
Each approach has its advantages and disadvantages. They also depend on the experience of surgical teams.

The patient remains in the recovery room for about 2 hours. The anaesthetist adjusts an analgesic treatment by venous route.
A urinary catheter is placed for a few days.
A treatment to avoid phlebitis is introduced by daily subcutaneous injection.
Hospitalization lasts between 2 and 4 days.
When you leave, a pain treatment is prescribed, nursing care every 2 days will be set up. Physiotherapy sessions can be started within 2 months.
You should avoid carrying heavy loads (more than 5 kg) for about 3 weeks.
After a hysterectomy, sexual intercourse is not recommended for 6 weeks.
Extended travel by car, train or plane is not recommended for about 10 days.
Driving is often possible after 2 to 3 days for laparoscopic procedures (for short trips), after 14 days for vaginal operations and after 21 days for laparotomy.
Sports activities are not recommended and are reassessed by your surgeon. After laparotomy, a 30 to 60 minute walk or swimming is possible after 2 to 3 weeks and violent sports after 6 weeks.
You will see the surgeon again at 1 week
Any additional questions? Ask your MEDICAIM doctor about it: careteam@medicaim.com
Some needs and conditions are more complex than others. In case of doubt, please send us additional information to establish a customized quote.
Ask for a quoteCertains besoins et pathologies sont plus complexes que d’autres. En cas de doute, faîtes-nous parvenir des informations complémentaires pour établir un devis sur-mesure.
Demander un devisEntrust us with your medical file and it will be examined by a specialist doctor. The goal?
Allow you to evaluate all your treatment options.